
This Article From Issue
January-February 2012
Volume 100, Number 1
Page 73
DOI: 10.1511/2012.94.73
THINKING, FAST AND SLOW. Daniel Kahneman. x + 499 pp. Farrar, Straus and Giroux, 2011. $30.
Did you know that highly intelligent women tend to marry men who are less intelligent than they are? This fact may appear to be a fascinating piece of information that reveals something about the socialization of women in our society, but it is actually a necessary consequence of statistics; it must be true. As long as the correlation between the intelligence scores of spouses is less than perfect, then if you have a very high IQ score, your partner is more likely than not to have a lower one, because most people have a lower one. No alternative explanation is needed.
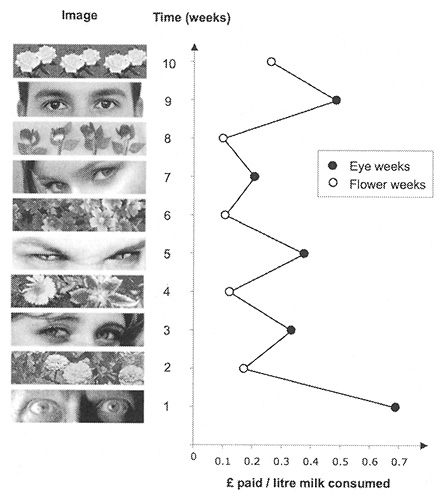
From Thinking, Fast and Slow.
Daniel Kahneman’s new book, Thinking, Fast and Slow, isn’t about marriage, IQ or the battle of the sexes. It’s about the battle that goes on inside us between a self that reacts quickly and automatically to fascinating facts, angry faces, tempting food and simple problems (what is 5 + 4?) versus a self that thinks more slowly, effortfully, and deliberately, explains facts by appealing to such things as the implications of random variation, tells us why people are angry and why we should resist temptation, and solves complex problems (what is 287+736?). These two selves make it possible for us to come to conclusions quickly when the need arises (should I hit the brakes or the accelerator?) and to slowly think through difficult decisions when many competing considerations must be weighed (should I buy an SUV or a minivan?).
For psychologists who want to understand how the mind works, slow thinking tends to be easier to explain. People generally have some insight into their slow thought processes. They can to some extent introspect and articulate what they were thinking.
We are less conscious of what goes on under the hood when we are thinking fast. What is the process you used to conclude that 5+4=9? It must have something to do with memory, but presumably you didn’t appeal to any specific memory. You recognized an abstract pattern and completed it. Psychologists have only vague ideas about how we represent such abstract patterns and reason about them so quickly and effectively. We do know that the mind brings a lot to the table. The conclusions we come to with such speed and automaticity meet our needs the vast majority of the time, yet they are not consistently optimal. The mind produces systematic errors. One reason for this is that fast thinking is shaped not only by the world being thought about, but also by the way the mind goes about its business.
The focus of Kahneman’s book is characterization of this process of rapid thought. In a masterly fashion he has woven several strands of insight into a finely detailed tapestry. Much of what he reports is an updated version of the work he did with Amos Tversky in the 1970s and 1980s—work that constitutes one of the great intellectual achievements of the 20th century—and the work for which he was awarded the Nobel Prize in Economic Sciences in 2002. The names Kahneman and Tversky are almost synonymous with the study of judgment and decision making—the study of how human psychology operates under conditions of uncertainty and the biases that result, biases that cause us to get less of what we want, be it love, money, health or merely accuracy. Their work is important because of what it teaches us about how the mind works and also because it offers numerous hints about how we can do better, both as individuals and as a society. It challenges the idea, pervasive in economics, that people have consistent preferences that guide their choices. Rather, Kahneman says, “inconsistency is built into the design of our minds,” as every clinical psychologist already knows.
Kahneman refers to the two selves simply as System 1 and System 2. This is unfortunate, as there are perfectly good English words to describe the mental systems he’s trying to characterize: intuition (fast thinking) and deliberation (slow thinking), for instance. This is not his only odd choice of labels. He calls one of his primary principles of intuition WYSIATI (What You See Is All There Is). Although the acronym is not mellifluous, the underlying concept—that we humans have a tendency to focus only on what is staring us in the face—is important. One implication is that we jump to conclusions on the basis of limited evidence. Other consequences of this tendency of ours are more subtle. For instance, you can have a profound effect on how people rate their overall happiness simply by first asking them, “How many dates did you have last month?” People will attend to the quality of their dating life (good, bad or indifferent) and use it as a basis for evaluating their well-being in general. Similarly, data show that, contrary to what Midwesterners and Californians believe, people in California are not in fact any happier than people in the Midwest. Kahneman attributes this to our tendency to answer questions with whatever happens to be in our minds. When asked whether Californians are happier, people (even Californians) think about sunshine and celebrities. But actual life in California is much like life elsewhere—filled with daily commutes, office parties and too much time spent watching TV. And it’s actual life that determines happiness, not the image that happens to come to mind when answering a question.
Another consequence of WYSIATI is that we evaluate events that actually happened without considering alternatives. In the face of evidence, we are more concerned with how good a story we can tell about it than we are with coming up with alternative accounts to explain it, remembering other events that contradict it, or thinking about how things might have been otherwise. Ask any good lawyer or politician stumping for votes. Wrapping events into a good story that supports one’s case is far more persuasive than poking holes in somebody else’s story or making a fair and balanced argument. Governments are evaluated by the actual state of the economy, not by how good or bad the economy would have been if some other policy had been in place.
Most of the territory the book covers is well trodden. But for the uninitiated, the book is a treasure trove of insights about the human condition. Kahneman goes well beyond discussing the primacy of intuition and how we make sense of events using causal stories. He explains that intuition is governed by a normality principle: Thought and perception are always interpreting what is in the focus of attention relative to a background that reflects what we consider to be normal. Feelings of surprise, guilt and blame all depend on how normal an action or event is. Kahneman uses this idea to explain why most people see nothing amiss with the following question: “How many animals of each kind did Moses take into the ark?” Of course, Moses didn’t take any animals into the ark; Noah did. Yet Moses fits into the biblical context—he seems normal there—and so most people fail to register the discordance. As Kahneman points out, if Moses were replaced in the question by George W. Bush, everyone would notice.
Kahneman and Tversky’s work changed the face of social and cognitive psychology and had a massive influence in economics and other social-science disciplines. Their work served as perhaps the most central intellectual antecedent of libertarian paternalism, the philosophy espoused by Richard H. Thaler and Cass R. Sunstein in their 2008 book, Nudge. Libertarian paternalism is the view that, because the way options are presented to citizens affects what they choose, society should present options in a way that “nudges” our intuitive selves to make choices that are more consistent with what our more deliberative selves would have chosen if they were in control.
Kahneman has kept abreast of developments in social psychology, economics and social policy. His discussion of cognition is less up-to-date, however, and even a little confusing. For instance, he makes it clear that he considers the two systems of thought to be a fiction, useful for didactic purposes only. This seems to undermine the book’s foundation and makes it hard to know what he is really saying about the architecture of the mind.
Kahneman and Tversky practiced what Kahneman here preaches. They made sound arguments, but they also knew how to tell a good story fluently and succinctly, in an engaging, punchy style. Thinking, Fast and Slow is not as succinct, but it is certainly fluent. It is chock-full of fascinating and provocative examples that reveal aspects of ourselves that we knew at some level existed but had not fully appreciated. The book appeals not only to our deliberative selves, but to our intuitive selves as well.
Steven Sloman is a professor in the Department of Cognitive, Linguistic, and Psychological Sciences at Brown University. His research interests include causal reasoning, decision making and categorization.

American Scientist Comments and Discussion
To discuss our articles or comment on them, please share them and tag American Scientist on social media platforms. Here are links to our profiles on Twitter, Facebook, and LinkedIn.
If we re-share your post, we will moderate comments/discussion following our comments policy.