The Merritt Parkway and Other Driving Respites
By Henry Petroski
Smaller roads offer an escape from the strangled traffic of I-95, as well as a detour into the pre-interstate highway era of automobile travel.
Smaller roads offer an escape from the strangled traffic of I-95, as well as a detour into the pre-interstate highway era of automobile travel.

DOI: 10.1511/2016.119.86
Interstate 95, the infamous East Coast superhighway that runs between Miami, Florida, and the U.S.-Canadian border in northeastern Maine, has a well-deserved reputation for heavy traffic thick with tractor-trailers. My wife and I drive a good deal on this road, and we welcome chances to escape running with the big rigs. Driving north from North Carolina, our first opportunity to do so comes at Washington, DC, where it is possible leave I-95 and drive for about 30 miles on the Baltimore-Washington Parkway, from which commercial traffic is prohibited. Thank goodness for parkways, with their grassy shoulders and abundance of trees.
But then it is back to jockeying with the truckers. A partial respite comes on the portion of I-95 that is coincident with the New Jersey Turnpike. Just south of the Pennsylvania Turnpike exit, the roadway divides into two sets of lanes, the inner of which are for automobiles only, but the trucks are never out of sight. There is also a way to escape trucks altogether, at least for a time, by leaving the Jersey Turnpike at exit 11 and continuing north on the Garden State Parkway. Unfortunately, the volume of automobile traffic on this road during rush hour can lead to slow if not stop-and-go traffic.
After running 40 or so miles through northern New Jersey on the Garden State, the parkway ends at the New York state line. The continuation road joins the usually crowded New York State Thruway, which crosses the Hudson River via the aging Tappan Zee Bridge ( see this column in the May–June 2012 issue ), whose replacement is currently under construction. Although the traffic—ranging from motorcycles to 18-wheelers—can proceed at a crawl through this bottleneck, there is soon an opportunity to get off the interstate and onto another road from which trucks are banned: the Hutchinson River Parkway, known by locals as “the Hutch.” It is one of the many parkways influenced by the urban planner Robert Moses, who has been described variously as a “master builder” and a “power broker” when it comes to roads, bridges, and parks built in and around New York City in the mid-20th century.
The Hutchinson River Parkway runs from the southeastern corner of the New York City borough of the Bronx northerly through that borough and on through Westchester County. Construction of the Hutch began in 1924 and, like a lot of roads, was completed in stages, the first two-mile section opening in late 1927. Ten years later the parkway reached the Connecticut state line, but it was clear long before then that a continuation of the parkway into Connecticut was all but inevitable.
The 1920s had brought tremendous growth in automobile ownership, but good roads lagged. The Lower Boston Post Road, which became U.S. Route 1 when the national highway numbering system was established in 1926, was carrying increasing volumes of traffic through communities along the north shore of Long Island Sound; congestion there was becoming intolerable. A controlled-access highway running parallel to Route 1 but located inland would go a long way towards alleviating the problem for Connecticut drivers and for those passing through on their way to and from New York City. Talk about the Route 1 problem began in the early 1920s, but the parallel-relief-road solution took more than a decade to become reality.
Because it would be a continuation of the Hutchinson River Parkway, the new highway’s westernmost location had to pass through Connecticut’s Fairfield County, which was the state’s most populous, affluent, and politically influential. In 1924, in anticipation of the new road, the Fairfield County Planning Association (FCPA) was formed as an advocate for preserving the county’s physical beauty and historical setting. Not incidentally, it was also intended to preserve land values and be vigilant about the threat of New Yorkers coming into the county, acquiring land to develop, and changing its character. The FCPA would exert a strong influence on the nature and design of the planned parkway.
Every major road needs a champion, and in Connecticut it was Yale-educated Schuyler Merritt, a Republican member of the U.S. House of Representatives and also a member of the FCPA. It seemed to be a given that the new road would be named after Merritt, but would its surname be Boulevard, Highway, or Parkway? The term boulevard , etymologically rooted in the French and German military terms for rampart and bulwark, had negative connotations for other reasons as well, because it implied an open road along which drivers sped unimpeded to the suburbs while cross traffic was halted at stop signs. Highway was such a generic term that it had to be qualified to tell whether it was limited access. The term parkway generally implied limited access, and it carried the further implication that it was a nicely landscaped road hidden from outside view and closed to commercial traffic.
In the early stages of planning, the future alternate route to the Boston Post Road was commonly referred to as Merritt Boulevard, a designation that John Macdonald, the state highway commissioner, did not favor. At one point he stated that the time to the road’s being a reality would be shortened if the people of Fairfield County through which it would run “would stop calling it a boulevard.” Legislation began to refer to the new road as the Merritt Highway, but by the time design and construction began there would be no question that it was really going to be a world-class parkway.
Before construction could begin, Macdonald had to find a way to acquire land for a right-of-way that was 300 feet wide along the length of the parkway. Initially, the Merritt was expected to parallel the Post Road for almost 20 miles and then turn south to join it. According to one account, in some areas the state highway department was considering as many as eight alternative routes, and the secretive Macdonald did not share them with the public or even with politicians. This action may have been taken to avoid land speculation, but it did not prevent corruption.
Rather than acquire the necessary land through the state’s right of eminent domain, Macdonald established a system whereby land was bought for a price negotiated by a special purchasing agent. That job went to a former state assemblyman and real estate broker named G. Leroy Kemp, who supplemented his modest salary with kickbacks from other brokers. When it came to light that Kemp, who necessarily knew the exact route of the parkway, was acquiring parcels of land for much more money than their assessed value, the scam was ended and Macdonald was forced to resign as head of the highway department.
Macdonald’s secrecy about the alignment of the parkway had inadvertently made graft possible when he put Kemp in charge of making land deals. It was also Macdonald’s style to give his engineers and architects leeway in designing the parkway’s road, bridges, and landscaping—as long as they adhered to his overarching principles, which tended to emphasize function over form. However, the generally young staff was bright and talented and would likely have worked well together regardless. After Macdonald resigned, the engineers and architects were able to recast the design into one that balanced function and form, or even gave the advantage to the latter.
One constant in the design of the Merritt Parkway as it evolved was the 300-foot-wide right-of-way. This area was to be equally divided into 150-foot-wide strips, with the northern one to be used for the new road. (The other strip was reserved for unspecified future expansion, the nature of which would be hotly debated in later decades.) The parkway was built during the Depression, so keeping costs down was an overarching objective. One way of doing so was to build overpass bridges with as short a span as possible. A minimum span of about 80 feet might have been determined by the fact that the parkway was to have two lanes in each direction, generally separated by a 21-foot-wide median.

As late as February 1936, the details of a final parkway plan were not in place, as evidenced by the response of Warren Creamer, chief field engineer for the project. When asked if the width of the median would be uniform, he replied, “I don’t know . . . the Commissioner hasn’t given a definite opinion on that yet. It may be varied.” And indeed it was. By tapering the width of the median down to 16 inches as the roadway went under overpasses, spans as short as 60 feet could be used. This resulted in “pinched bridges,” which meant that traffic in each direction ran close to the abutment wall on its right, and to the narrow median and oncoming traffic on its left. Creamer’s response also confirmed the idea that Macdonald had had the final say, as long as he was in charge.
The engineer responsible for the structural design of the parkway’s overpasses and underpasses, most of which were based on a common steel frame, was Leslie G. Sumner. Despite the shared underlying structure, Sumner’s goal was not to seek undistinguished uniformity, for he believed that extra money should be spent on aesthetic finishes when a highway “passes through country of some natural beauty which should not be marred by the more unfortunate works of man.” The commonality of the underlying structural design was well disguised by the concrete coverings that made each bridge appear to be unique. Facing the bridges in stone, as had been done on the Hutchinson River and many other early parkways, was considered too expensive, and only three of the Merritt Parkway’s bridges were so finished, one being the granite-faced arch over the Rippowam River, which the famed sculptor Gutzon Borglum could see from his property. At the time, his clout derived from his monumental work on the face of Stone Mountain, Georgia, rather than on his later masterpiece on Mount Rushmore.
The parkway was an immediate hit. Swiss architecture critic Sigfried Giedion called it "a master piece of organic layout."
The more familiar Merritt Parkway bridges were given a variety of sculptural, color, and textural finishings. Those treatments were designed by George Dunkelberger, who had trained in architecture at Philadelphia’s Drexel Institute. After World War I he and a partner opened a practice, but the Depression forced Dunkelberger to seek other work. He found it with the Connecticut Highway Department, which he joined in 1933 as a junior draftsman. In time, he became responsible for the signature designs of 37 of the parkway’s overpasses and 35 of its underpasses.
There was also the matter of landscaping, which (initially at least), according to Creamer, was “to assist nature in hiding the scars of construction.” Macdonald had put engineer A. Earl Wood in charge of the highway department’s Bureau of Roadside Development, among whose goals were contributing to highway safety, lowering maintenance costs, increasing the value of abutting property, and promoting Connecticut’s beauty. Wood understood that he himself was not a landscape architect, but he recognized the talent of one in Weld Thayer Chase, who was given responsibility for all of the Merritt’s landscaping. Even Macdonald, who initially had set aside a total of $250,000 for landscaping, admitted in response to a question that more than 10 times that amount should be spent “to retain the natural appearance of the county.”
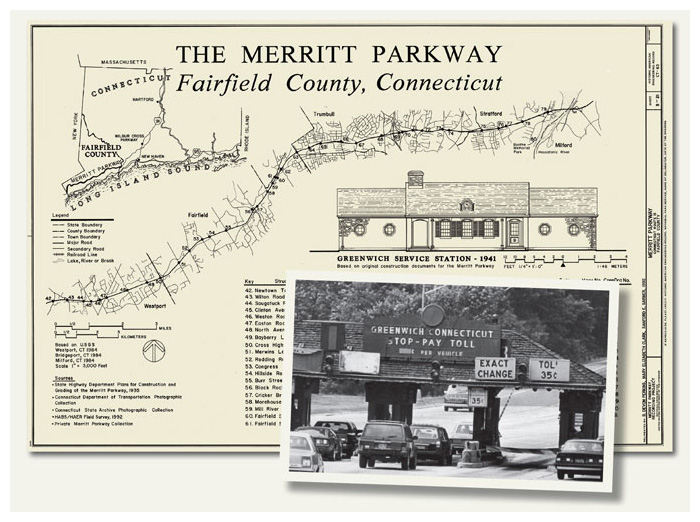
The first section of the Merritt Parkway—a 17-mile stretch from Greenwich, on the New York state line, to Norwalk, Connecticut—was opened in mid-1938; the second section—about 15 miles, to Trumbull—in late 1939; and the last—completing all 37.5 miles to Stratford, on the Housatonic River—in 1940. The total cost has been variously reported as being between about $22 million and about $32 million, depending on what is included. The Swiss architecture critic Sigfried Giedion called the Merritt “a masterpiece of organic layout exemplifying the arrangement of the modern parkway,” and the historian and philosopher of technology Lewis Mumford praised its civilizing effect on mechanization.
The parkway was an immediate hit with commuters and pleasure drivers alike, but it had its detractors. The critic Elizabeth Mock, who directed the department of architecture and design at New York’s Museum of Modern Art, called the ornament on the bridges “vulgar,” and Gilmore Clarke, designer of the pioneering Bronx River Parkway—the first highway to be built through a park, the first to employ a median between opposing lanes of traffic, and the first to use overpasses for intersecting roads—declared the Merritt “out of date before it was built.” Clarke may have been expressing sour grapes for not having been hired to design the Merritt or even being retained as a consultant, but the fact that all of the design work was done within the Connecticut Highway Department was one of the parkway project’s distinguishing characteristics.
The continuation of the Merritt Parkway beyond the Housatonic River is known as the Wilbur Cross Parkway, named for the Connecticut governor who was in office during much of the time that the Merritt was being built. The first section of the Wilbur Cross, about six miles long from Milford on the east bank of the Housatonic to Connecticut Route 34, opened in 1941. World War II interrupted its construction; when work resumed, the remainder of the 25-mile-long road to Wallingford was completed in two stages, opening in 1947 and 1948. Today, the Wilbur Cross, which like the Merritt is designated Connecticut Route 15, runs all the way to Meriden. Until 1988, both the Merritt Parkway and the Wilbur Cross were toll roads.
Among the legitimate criticisms of the Merritt and other parkways of the 1920s and 1930s were their short entrance and exit ramps, making joining and leaving the traffic flow very dicey. Even with today’s faster-accelerating cars, getting onto and off of the road can be nerve-wracking. The presence of stop signs rather than yield signs at the end of some entrance ramps makes merging into speeding traffic all the more difficult. It was not long before the standards of extended exit and entrance lanes set for interstate highways made the parkway’s constricted conditions all the more noticeable. But even with its shortcomings, the Merritt and other parkways proved their value to commuters and weekend drivers alike. That is not to say that they completely relieved congested conditions in the region, though, for as fast as roads multiplied, the number of vehicles using them seemed to grow to fill them.
Connecticut drivers experienced some further relief when the Connecticut Thruway (Interstate 95) was dedicated in early 1958. Traffic volume on the parallel Merritt dropped by about a third, but by 1980 had returned to pre-I-95 levels and kept growing. This led the federal highway department, now known as the Department of Transportation, to look for ways to “improve” the Merritt. The original low wooden guardrails were replaced first with cables between the posts, then with the corrugated steel rails so common on interstates. Some of the Merritt’s interchanges were also made more user-friendly. These alterations made subtle differences in the appearance of the parkway; much more dramatic changes resulted from neglected maintenance of the signature landscaping and shoddy repairs made to deteriorating bridges. Furthermore, where some intersecting highways were widened, the original unique bridges that carried them over the Merritt were replaced by unadorned steel-girder spans that look just like those across just about every interstate highway.
The historical significance of the Merritt Parkway was recognized in 1991 when it was added to the National Register of Historic Places; its precarious future was acknowledged in 2010, when it was named one of America’s Most Endangered Historic Places by the National Trust for Historic Preservation. The ongoing erosion of the Merritt’s most distinguishing features had already led to the establishment in 2002 of the Merritt Parkway Conservancy, which is dedicated to the protection and preservation of the parkway’s original character and integrity.
Tight budgets, lack of appreciation for the landmark’s historic significance, and apparent preference for function over form by the Connecticut transportation department had forced the conservancy into constant battles. In recent years, the department, aided by a combination of federal and state funding, has undertaken a series of projects “to provide safety improvements and enhancements” to the Merritt. Included in those efforts were improved roadway drainage, widened shoulders, steel-backed timber guardrails, and repair and rehabilitation work on about a dozen of the parkway’s signature bridges. But these pinched bridges will not be replaced. The repaved roadway will remain at its original width, an act of preservation that can be appreciated—or not—by every driver passing along the parkway.
I am grateful to Joel O. Lubenau, a regular user of the Merritt Parkway, who called my attention to the recent article by Herbert Newman and reignited my admiration for the parkway and its bridges.
Click "American Scientist" to access home page
American Scientist Comments and Discussion
To discuss our articles or comment on them, please share them and tag American Scientist on social media platforms. Here are links to our profiles on Twitter, Facebook, and LinkedIn.
If we re-share your post, we will moderate comments/discussion following our comments policy.