Slicing into the Past
By Felice Frankel
CT scans yield a three-dimensional image of a mummy's head
CT scans yield a three-dimensional image of a mummy's head

DOI: 10.1511/2006.62.550
Take a look—a careful look—and figure out what you are seeing. I am delighted to once again present a winning image from the Science and Engineering Visualization Challenge, sponsored by the journal Science and the U. S. National Science Foundation, where for the fourth year I am privileged to be a judge. The moment this image came on the screen, we all sighed with wonder. We're seeing the head region of a 2,000-year-old mummy of an Egyptian child (notice the head within the cartonnage?) from the Rosicrucian Egyptian Museum in San Jose, California. The detail is part of a larger three-dimensional image reconstructed from 60,000 exceptionally high-resolution two-dimensional scans, made without disturbing the fragile mummy-case. The team was led by endodontist W. Paul Brown of the Stanford-NASA National Biocomputation Center, working with physicist Rebecca Fahrig in the Department of Radiology and other colleagues at the Stanford University School of Medicine.
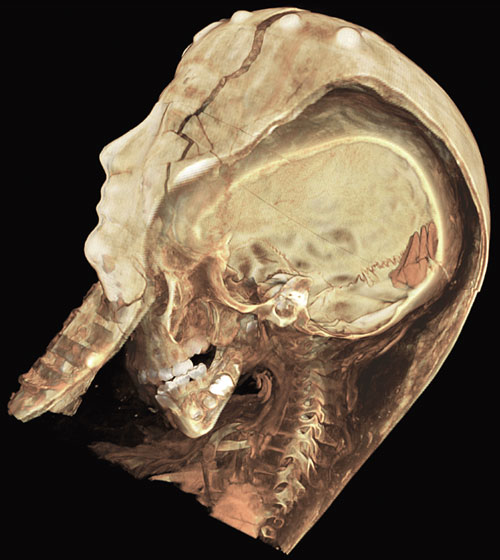
F. F. Paul, tell us how your team created the final image.
W. P. B. A team of physicists and radiologists at Stanford used a Siemens AXIOM C-arm CT scanner to generate 2-D slices about 200 microns thick, considerably thinner than the 750-micron slices used to create the 3-D visualization of King Tut's mummy. Robert Cheng, Eric Herbranson, Christof Reinhart, Juel Herbranson, Kevin Montgomery, Afshad Mistri and Amy Ladd used Volume Graphics' real-time ray-tracing technology to render and visualize the data set on a Silicon Graphics Prism workstation for the creation of the 3-D models.
F. F. What sort of information about the mummy did you discover?
W. P. B. From a series of detailed studies, we arrived at the following conclusions: The mummy was a female, between the ages of four and five years old, who probably died from a common intestinal illness or other disease, since we found no signs of injury (half of all Egyptian children died before their fifth year). Her family was probably wealthy—a scented resin was applied on the golden face mask.
F. F. The CT scans are grayscale, but the final image is colored.
W. P. B. Yes, we colored the image based on tissue density, thus making the teeth white (high calcium/highest density) and the bones a light sort of bone color, and finally applying reddish tints to the soft tissue.
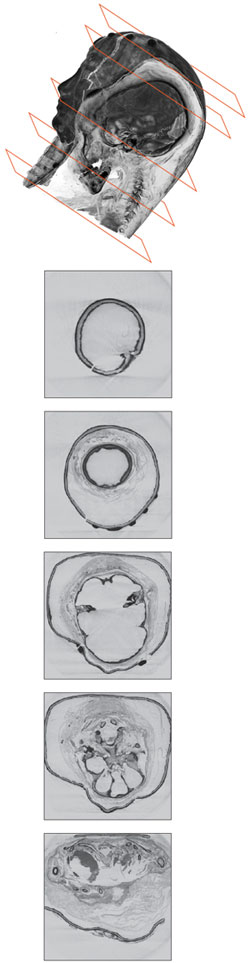
Images by Robert Cheng, courtesy of Brown & Herbranson Imaging; top diagram by Barbara Aulicino.
F. F. Can you tell us how the ray-tracing software was used?
W. P. B. To make a cutaway that has depth information, you need to cast a virtual light on the interior structures to create shadows and contrasts. This would be the job of the Volume Graphics package.
F. F. Can you imagine how these sorts of efforts might advance our understanding of those of us who have not yet been mummified?
W. P. B. Well, I would say that advances in high-resolution scanning and visualization technology are already transforming educational programs and medical procedures. As a dentist, I certainly see a change in orthodontic, endodontic and implant studies. I think the ability to interact with virtual anatomical information without invasive procedures can only enhance our efforts in understanding our own anatomy and will help to guide nonsurgical medical interventions.
Click "American Scientist" to access home page
American Scientist Comments and Discussion
To discuss our articles or comment on them, please share them and tag American Scientist on social media platforms. Here are links to our profiles on Twitter, Facebook, and LinkedIn.
If we re-share your post, we will moderate comments/discussion following our comments policy.